Home / Publications / Intelligence Memos / How AI is Helping with Physician Paperwork and Why We Need to Do More
- Media Releases
- Intelligence Memos
- |
How AI is Helping with Physician Paperwork and Why We Need to Do More
Summary:
| Citation | Tingting Zhang. 2026. How AI is Helping with Physician Paperwork and Why We Need to Do More. Intelligence Memos. Toronto: C.D. Howe Institute. |
| Page Title: | How AI is Helping with Physician Paperwork and Why We Need to Do More – C.D. Howe Institute |
| Article Title: | How AI is Helping with Physician Paperwork and Why We Need to Do More |
| URL: | https://cdhowe.org/publication/how-ai-is-helping-with-physician-paperwork-and-why-we-need-to-do-more/ |
| Published Date: | April 23, 2026 |
| Accessed Date: | June 3, 2026 |
Outline
Outline
Authors
Related Topics
Files
For all media inquiries, including requests for reports or interviews:
From: Tingting Zhang
To: Health system observers
Date: April 23, 2026
Re: How AI is Helping with Physician Paperwork and Why We Need to Do More
Ask a family physician what frustrates them most, and it’s rarely about medicine. It’s the paperwork.
Referrals, insurance forms, and electronic documentation – the administrative tasks that consume hours every week and divert their time from direct patient care. For Canadian physicians already stretched thin, this hidden workload is exhausting.
New data from the 2025 Commonwealth Fund (CMWF) survey reveals a mixed picture: Encouraging progress alongside persistent challenges.
There’s reason for cautious optimism. Compared to 2022, a lower proportion of physicians is unhappy with their administrative workload across most surveyed countries. Canada, Australia, and New Zealand saw the largest drops – each falling 20 to 28 percentage points. The CMWF average fell 18 percent.
However, nearly two in five Canadian family physicians still report burnout, second only to the United States. In some provinces, the situation is even more acute: As many as two-thirds of physicians in PEI are affected. This burnout carries real costs: $213 million tied to early retirements and reduced clinical hours a decade ago, a figure that has certainly grown. Among the leading causes of burnout, half of Canadian family physicians identify administrative tasks as the primary source of strain.
The most burdensome tasks, cited by about three-quarters of respondents, include referrals and test requisitions, insurance paperwork, and electronic documentation. On average, Canadian family physicians spend 10 hours per week on administrative tasks, about half of which is unnecessary. Nationally, those unnecessary tasks represent roughly 19.8 million wasted hours every year. In other words, dissatisfaction has declined, but the underlying problem persists.
Meanwhile, AI has been helping. Scribe tools can record and transcribe clinical encounters, generating clinical documentation that clinicians can review, edit, and sign. Canada Health Infoway launched the AI scribe program last year, providing more than 10,000 primary care clinicians with a fully funded, one-year AI scribe licence. As of last August, 9.2 percent of family physicians are actively using these tools. Preliminary findings suggest that they save five to 20 minutes per patient per day.
More rigorous studies show modest but durable reductions in documentation time, ranging from seven to 22 minutes per day post-encounter, depending on specialty and workflow. The Permanente Medical Group found that over a year of use, AI scribes saved more than 15,700 hours for users compared with nonusers, equivalent to 1,794 working days, among 7,260 physicians.
Beyond time savings, multiple studies show that AI scribes reduce burnout, lessen after-hours clerical work, improve cognitive load and enhance physician-patient interaction.
Canada’s adoption rate is notable. In 2025, Canada ranked second among CMWF countries in the share of physicians using AI in some capacity (46 percent) – whether for clinical, administrative, or other tasks, just behind New Zealand (55 percent). For notetaking specifically, 68 percent of Canadian physicians with access to AI scribes use them frequently, well above the CWMF average of 45 percent (Figure). New Brunswick leads the country, with four in five physicians using this technology.
However, AI scribes only address one slice of the administrative burden. They save time on electronic documentation, but do little to ease other tasks such as referrals, insurance forms and billings.
Compared with other Commonwealth Fund countries, Canada is less likely to use AI for billing or clinical decision support (Figure), highlighting a significant untapped opportunity. AI can automate billing code extraction, complete standardized forms such as disability and insurance paperwork, and augment clinical decision-making by flagging drug interactions, recommending specialist referrals, and suggesting diagnostic tests. The goal is to enhance, not replace, physician judgment.
To realize these benefits at scale, governments need to promote wider engagement among non-users, vet vendors, and provide training and ongoing support to ensure that physicians can effectively leverage these tools. Broader adoption will improve the return on investment and help unlock productivity gains. At the same time, risks related to accuracy, privacy, ethical use, and workflow integration must be carefully managed.
While technology can help, governments should also focus on practical reforms such as harmonizing and simplifying insurance forms, improving billing procedures, and ensuring that basic information, such as specialist wait lists, is accessible to patients and physicians. The most effective approach to reducing administrative burden combines both: Using technology where it adds value and simplifying processes where it matters most.
Reducing administrative burden frees physicians to do what they entered medicine to do: Care for patients. This improves physician wellbeing, reduces burnout, lowers early retirement rates, and ultimately strengthens primary care access and quality.
Canada should act now to maximize the benefits of AI for both patients and physicians. The technology works. The question is whether we have the will to implement it properly.
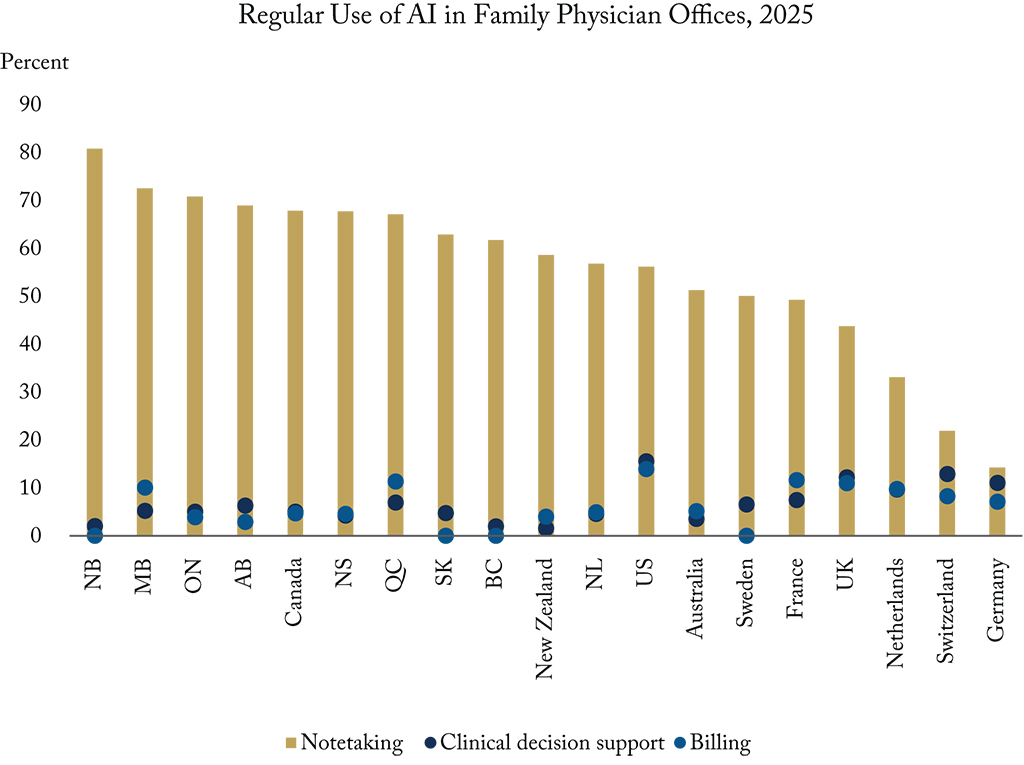

Note: The indicator includes office practices with access to AI tools and reflects those who report using them usually or often.
Source: The Commonwealth Fund, 2025 International Health Policy Survey of Primary Care Physicians.
Tingting Zhang is a Policy Analyst at the C.D. Howe Institute.
To send a comment or leave feedback, email us at blog@cdhowe.org.
The views expressed here are those of the author. The C.D. Howe Institute does not take corporate positions on policy matters.
Related Publications
- Intelligence Memos
- Intelligence Memos

